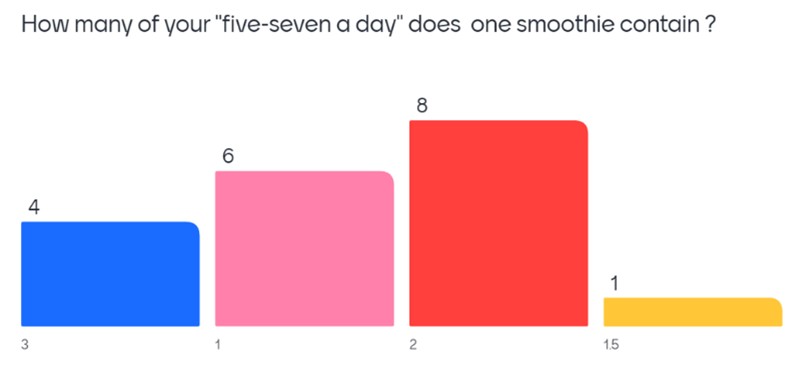21 April, 2026
I recently presented on nutrition and narcolepsy at a Narcolepsy Information and Support Event for patients attending the National Adult Narcolepsy Service at St. James’s Hospital.
More than 25 patients attended. Alongside nutrition, the event covered stigma and social support, treatment updates, coping with the impact of narcolepsy on thinking, behaviour and memory, and a panel discussion on challenges and coping strategies.
The discussion reinforced an important point for me: narcolepsy affects more than sleep. It affects routine, eating, movement, confidence, cognition, and quality of life. That is why multidisciplinary care matters.
From a dietetic perspective, one of the main challenges is the disruption narcolepsy can cause to eating patterns. Frequent waking during the night can lead to late-night eating, which can become difficult to manage and may contribute to weight gain. At the same time, strategies used to manage narcolepsy, such as scheduled daytime naps, can reduce daytime intake. As a result, people may become hungrier later in the day and, when tired, may be more inclined to choose quick and convenient sugary snacks.
In practice, this means the issue is often not only what someone is eating, but when they are eating and how consistent their intake is across the day. Supporting a more regular meal pattern can be an important first step.
Another challenge is that patients may change their eating habits to manage symptoms. Some reduce carbohydrates to avoid post-meal tiredness, but this can lead to lower intakes of fibre, vitamins, and minerals. Others struggle with poor satiety and cravings for sweet foods. These are practical issues, but they also show why nutrition cannot be considered in isolation from the wider experience of living with a long-term condition.
Weight management can also be particularly difficult. Excessive daytime sleepiness can affect shopping, cooking, and meal preparation. Lower energy levels can make physical activity harder. For people living with narcolepsy type 1, cataplexy, a sudden loss of muscle tone triggered by strong emotions, may add another barrier, especially if there is concern about exercising independently.
These realities call for realistic, person-centred advice. In dietetic assessment, the focus is often on sustainable health behaviour change and goals that are achievable for the individual. That tends to support better conversations and more meaningful progress.
During the event, I used Mentimeter to make the session interactive. Patients responded to questions on their phones, which helped open discussion and challenge common nutrition myths. It also brought the focus back to practical, manageable changes rather than perfection.
For me, that was one of the most useful aspects of the day. Hearing directly from patients was a reminder that the challenges they face rarely sit neatly within one profession. Sleep, eating, movement, mood, cognition, and social support are closely linked. Events like this are valuable because they create space not only to share information, but also to reflect on how we, across HSCP disciplines, can contribute to care that is coordinated, practical, and centred on the person’s lived experience.